John’s Unexpected Childhood Diagnosis Leads to Lifelong Congenital Heart Care
When he was just 13 years old, John Gallegos had no idea he was living with a life-threatening congenital heart defect.


Top Surgical Outcomes in North America*
The Children’s Heart Institute at Children’s Memorial Hermann Hospital – named one of the top hospitals nationally in Cardiology & Heart Surgery by U.S. News & World Report – offers innovative solutions for patients with congenital or acquired heart disease. In collaboration with pediatric sub-specialists at McGovern Medical School at UTHealth, the affiliated team provides comprehensive care for newborns, children and adolescents, with a smooth transition into adult congenital cardiac care.
In addition, the Children’s Heart Institute ranks among the elite for congenital heart surgery programs in the United States and Canada, as evidenced by the most recent Congenital Heart Surgery Database (CHSD) report from the Society of Thoracic Surgeons (STS). The affiliated team continues to deliver high-quality outcomes, while providing personalized care to patients.
The Children’s Heart Institute partners with The Fetal Center at Children’s Memorial Hermann Hospital to offer patients with congenital heart defects (CHD) a complete range of prenatal testing and fetal interventions with a coordinated program for mother and child before, during and after birth. The Fetal Center is a national referral center and an international leader in fetal diagnosis, fetal intervention and comprehensive fetal care for infants with congenital anomalies or genetic abnormalities.
With the Level IV Neonatal Intensive Care Unit (NICU) and a dedicated pediatric Children’s Heart Institute Intensive Care Unit (CHI-ICU) at Children’s Memorial Hermann Hospital, critical pediatric heart patients have access to the highest level of specialized care. By utilizing state-of-the-art techniques and services, the Children’s Heart Institute strives to offer patients with the most complex problems the greatest opportunity for a healthy life.
Meet the team of affiliated physicians that provide comprehensive care to babies prior to birth, infants, and children with complex heart conditions.
Children’s Heart Institute publishes patient outcomes data in an effort to help families make informed decisions about their child’s care.
To best serve patients, online resources have been developed to educate families about specific complex congenital heart defects.

When he was just 13 years old, John Gallegos had no idea he was living with a life-threatening congenital heart defect.

This brave heart warrior already has undergone six heart procedures to address her complex condition: hypoplastic left heart syndrome (HLHS) with severely depressed heart function.

Diagnosed with Hurler-Scheie syndrome at just 10 years old, Rylee hasn’t had an easy journey, but her strength and positive attitude have never wavered through it all.
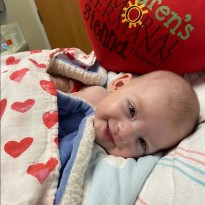
When Sienna Grace Wilson was born, a little fighter came into the world. Her parents, Sarah and David Wilson, were in awe of their new baby. They were also very emotional because of Sienna’s pre-birth diagnosis of Tetralogy of Fallot.

Amy and her team navigated through complex medical and emotional challenges with a level of courage, confidence and precision that saved her life and revitalized her future.

Navigating this amazing journey, Dottie’s parents, Brad and Caitlin, were by her side, backed by the medical team at Children’s Memorial Hermann Hospital where she was transferred after birth. From fetal heart diagnostics to the heart-wrenching uncertainties that followed, their daugh...

Their journey, however, took an unexpected and dramatic turn when, at just 22 weeks’ gestation, Jameka’s water broke prematurely. Fearing the worst, they rushed to a local Houston hospital where Jameka was admitted to the Labor & Delivery unit.

For Demetric Fisher, her daughter Kaydan's health was such a test. Born on June 20, 2012, in Jackson, Miss., little Kaydan’s life led her family on an emotional rollercoaster that would shape their lives for years to come.

Despite the previous reassuring tests, William’s position during the ultrasound raised concerns. His heart appeared too far to the left and his stomach couldn’t be located.
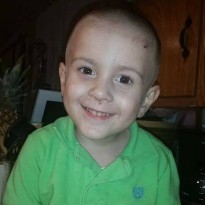
Shortly after Slade was born in October 2011, he was diagnosed with dilated cardiomyopathy. This condition is dominated by a heart that’s too big, causing the heart muscle to be very weak and have a leaky mitral valve.

As soon as possible, she and Troy made an appointment with The Fetal Center at Children Memorial Hermann Hospital for an in-utero echocardiogram, which would provide a detailed image of their baby's heart. Prenatal diagnosis plays a vital role in identifying critical cardiac defects, helps guide ...

Theodore was diagnosed with hypoplastic left heart syndrome (HLHS), a complex congenital heart defect in which the left side of the heart is underdeveloped and cannot pump oxygen-rich blood to the body. Babies with this condition need a minimum of three open-heart surgeries. ...

At the age of 5 months, Flora Sandt was already sitting and starting to roll, and she could push herself up on her belly and look around. She is the third child of Rebekkah and Justin Sandt, and based on their experience, she appeared to be meeting her developmental milestones. Then she caught a ...

When Falon was 23 weeks pregnant, she was very excited about her next ultrasound and couldn’t wait to catch a glimpse of Ryder on the ultrasound screen to see how much he had grown since his last anatomy scan. At first, things were going well. Then, the atmosphere in the room abruptly chan...

A passion for innovative solutions, a desire to provide hope to children who previously had none, outside-the-box thinking, and quality outcomes – these are the hallmarks of the Children’s Heart Institute, a collaboration between Children’s Memorial Hermann Hospital and McGovern Medical School at...

Sweet Isabella was held by her mother Jessica for just a few moments before being whisked away for her first heart surgery at just 14 hours old. Born with pulmonary atresia with intact ventricular septum, half of Isabella’s heart was severely underdeveloped causing major issues with blood f...

Rasheed Alshammari had been on the waiting list for a heart transplant at a California hospital for over a year. When the surgeon who was to perform the transplant left the hospital, Rasheed was removed from the list.

Karen and Taylor Mims spent the first six years of their son’s life trying to accept the fact that he was born with half a heart and would eventually require a heart transplant. Now, thanks to an innovative procedure being performed by affiliated pediatric heart surgeons at Children’s...

Kemberlee Burgert's baby was diagnosed with Ebstein anomaly, a rare congenital heart defect in which the tricuspid valve, the valve between the upper right chamber (right atrium) and the lower right chamber (right ventricle), isn’t formed properly, allowing blood to leak back into the right atriu...

At her 8-week maternity check-up, Chanelle Smith and her husband, Patrick, were surprised and delighted to learn that Chanelle was carrying identical twins. At 28 weeks, Dr. Ramos identified a small hole in the heart of one of the babies. Additional tests revealed that the baby suffered from a co...

During her 20-week ultrasound, Savannah’s obstetrician diagnosed that her unborn baby’s heart was abnormally small and referred her to a maternal fetal medicine specialist. The specialist ordered a dedicated fetal echocardiogram (“echo”), a specialized ultrasound of the fe...

A well-orchestrated chain of events saved the life of Caleb, a newborn with a rare and very serious congenital (present at birth) heart defect. Fortunately, that chain was populated by an experienced and collaborative team who worked together seamlessly to diagnose, transport and treat the baby. ...

Hayes appeared to be a perfectly healthy newborn. Three hours after birth, however, a nurse who was listening to his heart through a stethoscope heard an abnormal heart sound – a heart murmur – indicating a possible heart problem. A cardiologist ordered an echocardiogram (diagnostic cardiac ultra...

Erinn Brown was 34 weeks pregnant when she realized something was wrong with her baby. An ultrasound showed that the left ventricle of the baby’s heart was very small and nearly nonexistent. Brown’s doctor referred her to The Fetal Center at Children’s Memorial Hermann Hospital....

During a routine football practice Jordan suddenly felt dizzy and showed signs that something was wrong. He was immediately taken to Memorial Hermann where affiliated pediatric neurologist Dr. Ian Butler along with neurologist Dr. Nicole Gonzales diagnosed Jordan as having had a stroke. Later aft...
If you have any questions, use the online tool below to help us connect with you. To refer a patient or schedule an appointment, please contact our clinic using the information below.
To contact Children’s Heart Institute at Children’s Memorial Hermann Hospital, please fill out the form below.
If you are experiencing a medical emergency, call 911 or go to the nearest emergency room.
If you or someone you know needs support from the Suicide and Crisis Lifeline, call or text 988.
*According to the Fall 2019 Society of Thoracic Surgeons (STS) Congenital Heart Surgery Database Report of 118 STS participating programs.
The Children’s Heart Institute is a collaboration between the affiliated physicians at McGovern Medical School at UTHealth Houston and Children’s Memorial Hermann Hospital. Typically, patients are seen on an outpatient basis at a UT Physicians clinic with all inpatient procedures performed at Children’s Memorial Hermann Hospital.