Chase and Kendall Macek describe their son, Ripp, as a happy, wild and determined little boy. He loves hanging out on the farm and playing with his three big brothers, who he affectionately calls his “bubbas.” He loves trucks and tractors and enjoys helping his daddy with just about anything.
“He is daddy’s little helper for sure,” said Kendall. “When they were building his fort bed, Ripp used his toy drill to screw the bolts in. It was so cute to see them work together. Ripp is always ready to help, whether it’s working on the farm or doing a few small projects around the house.”
For the Maceks, their 22-month-old son, Ripp, is nothing short of a miracle.
 “If you see him today, you’d never know what he has been through,” said Kendall. “It’s hard to tell he was in a horrific accident. Pretty much everyone told us that God had his hand over his head.”
“If you see him today, you’d never know what he has been through,” said Kendall. “It’s hard to tell he was in a horrific accident. Pretty much everyone told us that God had his hand over his head.”
The Maceks credit the UTHealth Houston multidisciplinary trauma team affiliated with Children’s Memorial Hermann Hospital, and the rehabilitation team at TIRR Memorial Hermann for helping Ripp make a remarkable and complete recovery after sustaining six cranial fractures to his brain at just 14 months old.
A Freak Accident
On September 24, 2022, Chase and Kendall had a few friends over at their family farm in El Campo where they gathered around the fire pit, grilling fajitas. It was supposed to be a fun and relaxing afternoon on the farm. But then, in a matter of minutes, everything changed so quickly.Ripp had been run over by the family tractor. “Our older son was driving the tractor and he didn’t see his little brother,” said Chase. “When our son ran towards us holding Ripp in his arms, I will never forget Ripp’s distressed cry. He was in a lot of pain. He was bleeding profusely from his ear.”
Immediately, Kendall and Chase jumped in their truck and took Ripp to the emergency room which was a 15-minute drive from their home in El Campo. On the way there, Kendall, a former health care worker, tried to control the bleeding in his ear, stabilized his spine and kept him upright.
Once they got to the ER, the doctors ran a computed axial tomography (CT scan) on him. Moments later, they told the Maceks their son had a skull fracture, a brain bleed, and a broken spine, and he needed immediate surgery.
“They said Ripp could possibly end up as a quadriplegic,” said Kendall. “My husband and I were freaking out. Since this was not a pediatric care facility, and because of the serious injuries our son sustained from his accident, we requested Ripp be transferred to Children’s Memorial Hermann Hospital in the Texas Medical Center where we knew he would receive the best care possible.”
An hour later, Ripp was airlifted via Memorial Hermann Life Flight® to Children’s Memorial Hermann Hospital in Houston. As a Level I Pediatric Trauma Center, Children’s Memorial Hermann Hospital is equipped and ready to care for the most critical and severe cases. The transport team regularly transfers pediatric and neonatal patients from community hospitals, clinics and emergency centers when a higher level of care is required.
“When the Life Flight team got there, I fell to my knees,” said Kendall. “I could finally take a deep breath knowing our son was in good hands. The team intubated him before he was transported.”
A Higher Level of Trauma Care
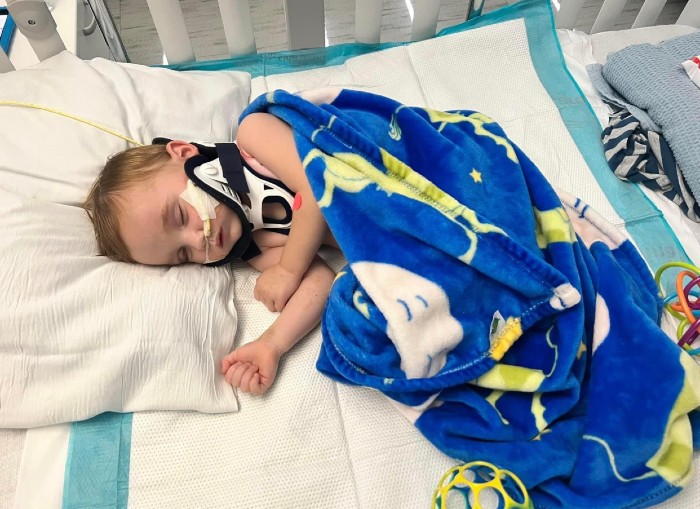 Ripp was critically ill when he arrived at the pediatric emergency room at Children’s Memorial Hermann Hospital. When the Maceks arrived, they met with multiple members of the trauma care team from McGovern Medical School at UTHealth Houston.
Ripp was critically ill when he arrived at the pediatric emergency room at Children’s Memorial Hermann Hospital. When the Maceks arrived, they met with multiple members of the trauma care team from McGovern Medical School at UTHealth Houston.
The affiliated multidisciplinary pediatric trauma team included general pediatric surgeons, emergency medicine, nurse practitioners and surgical residents and fellows. In addition, the trauma team also incorporated subspecialists such as pediatric neurosurgery and pediatric intensive care in Ripp’s case. Often when treating trauma patients, it takes the expertise of many subspecialties to ensure the best outcome for the child. Children’s Memorial Hermann Hospital is a certified Level I Trauma Center that can provide the highest level of trauma care available to children.
“When treating an acutely injured child, our primary focus is to stabilize and provide any immediate life-saving therapies,” said Dr. Kuojen Tsao, professor and chief of the Division of Pediatric General and Thoracic Surgery at UTHealth Houston and pediatric general surgeon affiliated with Children’s Memorial Hermann Hospital. “Through physical exam and advanced imaging, we were able to make the correct diagnosis and work on the appropriate treatment plan for Ripp.”
Ripp’s Diagnosis
Ripp had six cranial fractures with bleeding inside the skull. He also had a ligament injury to his cervical spine (neck sprain). Upon closer examination, Ripp also suffered a spinal hemorrhage and had hematomas (blood clots) in his transverse and dural venous sinuses, which are the vessels in the cranium that drain blood and cerebrospinal fluid circulating from the brain into the vascular system.
“Despite our son’s traumatic injuries, there was a silver lining too,” said Chase. “Since the blood and cerebral spinal fluid were draining from his ear, it prevented his brain from swelling so they didn’t have to do brain surgery to drain the fluids. However, his physicians were concerned about blood clots migrating to his spinal cord or entering his lungs. They were doing a bunch of tests and monitoring him closely and keeping him stable. We were also relieved to know Ripp did not have a broken spine as previously thought. He had a sprain in his cervical spine.”
While in the pediatric ER, Ripp was sedated and placed on a ventilator. Once he was stabilized in the ER, Ripp was admitted to the Pediatric Intensive Care Unit (PICU) at Children’s Memorial Hermann Hospital where Dr. Haitham Al Wahab oversaw his intensive care. Dr. Al Wahab is assistant professor of pediatric critical care medicine at UTHealth Houston and critical care medicine physician affiliated with Children’s Memorial Hermann Hospital.
Ripp was treated for other medical conditions in the PICU. He underwent two blood transfusions and was on a vasopressor (a medication to raise his blood pressure) for less than a day to help his blood pressure perfuse his spine adequately. Ripp received an anti-seizure medication to prevent seizures and his neurological status was monitored closely. Dr. Stephen Fletcher, professor of pediatric neurosurgery at UTHealth Houston and a pediatric neurosurgeon affiliated with Children’s Memorial Hermann Hospital, assessed Ripp’s cranial fractures and cervical ligament injury. Ripp wore a C-collar, or a neck brace, to support his head and to alleviate pressure on the ligaments in his neck.
The Plan of Care
While surgery wasn’t completely off the table, Ripp’s trauma care team recommended a wait-and-watch approach, which is typically used on patients with medical conditions that progress slowly.
“Not every brain injury or bleeding brain requires surgical intervention,” said Dr. Robert Lapus, associate professor at UTHealth Houston and affiliated medical director of the pediatric ER at Children’s Memorial Hermann Hospital. “Some injuries can be monitored for ongoing bleeding and swelling. Children lucky enough to avoid surgery still may have long-term concerns or issues that require the expertise of the specialists. The amazing thing about children is they often can heal themselves. Many of the injuries that Ripp sustained could heal on their own.”
“I remember the doctors telling us, ‘We are not going to do anything unless he absolutely needs it,’” said Kendall. “His entire care team involved us in daily rounds, which was really awesome. We never felt like we were out of the loop. They always included us in everything. We were involved in our son’s care and decision-making as much as his care team. They had a game plan for everything.”
Ripp spent seven days in the PICU and each day his condition gradually improved. After four days in the hospital, his ventilator was removed and replaced with a nasal cannula, a device that provides oxygen therapy through the nose, which he wore for a few days before he could breathe fully on his own. Ripp also had an NG tube for liquid feedings since he was sedated for several days.
“After he was taken off the ventilator, I got a chance to hold my baby,” said Kendall. “I wanted to do that the whole time. He was doing well and he didn’t need any surgical interventions at all.”
After seven days, the cerebral spinal fluid stopped leaking from his ear. His brain bleeds began to reabsorb into his body, and his skull fractures were gradually healing on their own. While in the hospital, he participated in physical and occupational therapies daily before starting pediatric rehabilitation therapy at TIRR Memorial Hermann.
Building Up His Strength
Following his traumatic brain injury, Ripp had to relearn everything — how to swallow, sit up, stand, walk and regain his overall muscle coordination. On October 10, 2022, he was transferred to TIRR Memorial Hermann where he began three weeks of physical, speech and occupational therapies. TIRR Memorial Hermann is designated as a national rehabilitation innovation center and offers comprehensive inpatient and outpatient care for patients with a life-altering injury or illness, such as a traumatic brain injury.
“Ripp was an ideal candidate for our program,” said Dr. Stacey Hall, assistant professor of pediatric rehabilitation medicine at UTHealth Houston and medical director of pediatric rehabilitation affiliated with TIRR Memorial Hermann. “At TIRR Memorial Hermann, we provide rehabilitation to patients with brain injuries of all levels of severity and are committed to helping them in their recovery. Given the severity of Ripp’s injuries, he looked better than we had anticipated. As an inpatient with us, he worked very hard. He progressed so quickly and his recovery was remarkable. Ripp was a resilient little warrior. He definitely captured our hearts.”
Ripp underwent five to seven hours of intense physical, occupational and speech therapies every day. As determined as their little boy was, he met all of his goals. By the time he left TIRR Memorial Hermann, Ripp could sit up and crawl. He could transition from standing up to sitting down to squatting. He could grasp objects better. His eye and hand coordination improved greatly and he was able to swallow thicker liquids. He was improving day by day until it was time to go home.
“His therapists, Emily (physical therapist), Taylor (occupational therapist) and Sabrina (speech language pathologist) at TIRR Memorial Hermann were amazing,” said Kendall. “When he left, he literally ran out of the hospital. I don’t know if I cried more when we got there or when we were leaving because everyone, including the patients, became family. Ripp would go through the hallways with his stroller and wave to everyone and blow kisses. Everyone was showing up to our unit to say goodbye to Ripp. Between Ripp’s doctors, nurses and Child Life specialists at Children’s Memorial Hermann Hospital and his entire therapy team at TIRR Memorial Hermann, everyone was professional and knew how to handle Ripp. Knowing your child is in good hands is the best thing in the world.”
 Ripp is doing great. He has follow-up appointments at UT Physicians clinics with Dr. Lupo and Dr. Fletcher to make sure his injuries are healing well. After three months of wearing a neck brace, he no longer needs one. His cervical ligament injury has improved. In addition to their son having a wonderful care team, the Maceks say their faith and support from family, friends and the community helped them get through this.
Ripp is doing great. He has follow-up appointments at UT Physicians clinics with Dr. Lupo and Dr. Fletcher to make sure his injuries are healing well. After three months of wearing a neck brace, he no longer needs one. His cervical ligament injury has improved. In addition to their son having a wonderful care team, the Maceks say their faith and support from family, friends and the community helped them get through this.
“As a parent, we are used to being in control, and in these situations, the only person who is really in control is God. He is going to put the right team in your child’s life and will guide you. Our best advice to other families is to stay positive, be hopeful, and rely on your faith to give you strength.
Visit Children’s Memorial Hermann Hospital’s Trauma Center for more information »
Contact Us
To contact Children’s Heart Institute at Children’s Memorial Hermann Hospital, please fill out the form below.
If you are experiencing a medical emergency, call 911 or go to the nearest emergency room.
If you or someone you know needs support from the Suicide and Crisis Lifeline, call or text 988.