 Steve Howell, 70, and his wife, Sharon, 64, once were avid triathlon athletes who trained together through running, swimming and biking near and far from their home in Katy, Texas. In 2016, Steve, then 60, was forced to retire from his job as a chemical engineer due to a company layoff. It was a change he didn’t see coming. It was also the beginning of subtle but concerning changes in his behavior and physical health.
Steve Howell, 70, and his wife, Sharon, 64, once were avid triathlon athletes who trained together through running, swimming and biking near and far from their home in Katy, Texas. In 2016, Steve, then 60, was forced to retire from his job as a chemical engineer due to a company layoff. It was a change he didn’t see coming. It was also the beginning of subtle but concerning changes in his behavior and physical health.
“I started to notice subtle changes in Steve’s personality and his actions after he retired,” Sharon said. “He stopped being interested in training with me. This was strange because this was central to our routine and social circle. He lost interest in a lot of things.”
For years, doctors attributed these symptoms to depression, possibly related to his forced retirement. But Sharon noticed something more. Steve had moments when he “just wasn’t himself,” along with occasional balance issues.
While Sharon trusted his doctors, she kept a close eye on Steve. In 2020, when COVID-19 hit, both of the couple’s sons moved back in with them. Their sons also noticed their dad was acting out of character—physically and emotionally—and sleeping more. Still, despite what Sharon called his “off days,” he was getting by, and there was no clear cause for alarm.
In retrospect, physicians later determined Steve was likely experiencing transient ischemic attacks (TIAs), often called “mini-strokes,” which are critical warning signs of a future major stroke.
Emergency Stroke Care at Memorial Hermann Katy Hospital: Recognizing the Signs
On July 17, 2022, those warning signs became a life-threatening emergency.
On that day, the couple hosted a family gathering to celebrate Sharon’s parents’ wedding anniversary. “We had a lot of people over, and they noticed Steve was much quieter than usual. He’s normally very social, but that day he kept to himself,” Sharon said.
After the guests left, Steve developed a severe headache. He took pain medication and went to nap. When he woke up, he was more disoriented. “He was talking but not making much sense and left the water running after washing his hands,” Sharon added.
He continued to complain of a headache. While a headache alone can be harmless, when combined with confusion and disorientation, it can signal a neurological emergency.
Recognizing these as potential stroke symptoms, Sharon acted quickly. She brought him to the Emergency Center at Memorial Hermann Katy Hospital, where the emergency team immediately initiated a comprehensive neurological evaluation.
“All the doctors and nurses…were so wonderful,” Sharon said. “They started examining him right away.”
Rapid imaging and stroke protocols revealed a cerebral venous sinus thrombosis (CVST). A rare and complex type of stroke that requires highly specialized care, a CVST is caused by a blood clot in the brain’s venous sinuses which can result in brain swelling and hemorrhage.
Advanced Stroke Treatment at Memorial Hermann-Texas Medical Center
As Steve’s condition escalated, he was transported to Memorial Hermann-Texas Medical Center via Memorial Hermann Life Flight®, utilizing the system’s integrated, rapid-response stroke network designed to connect patients to the highest level of care.
Aidan Azher, MD, assistant professor of Vascular Neurology at McGovern Medical School at UTHealth Houston and vascular neurologist affiliated with Memorial Hermann-Texas Medical Center, led his care.
The multidisciplinary stroke team used advanced neuroimaging, continuous monitoring and evidence-based protocols to manage a brain bleed caused by the clot, demonstrating the hospital’s capability and experience in treating complex cerebrovascular conditions.
“In complex stroke cases like Steve’s, rapid diagnosis and continuous neurological monitoring are critical to preventing further brain injury and guiding treatment decisions,” said Dr. Azher. “Our goal is to stabilize the patient and preserve as much neurological function as possible so they have the best chance at recovery through rehabilitation.”
“When Dr. Azher told me they weren’t going to have to open his skull, I finally calmed down a bit,” said Sharon. “Dr. Azher was so comforting. He told me Steve would likely be able to walk and talk after rehabilitation. It was such a relief to hear those words.”
During his time in the intensive care unit (ICU), Steve faced additional complications, including a risk of seizures, which are abnormal electrical activity in the brain that can worsen damage after a stroke. Doctors used medication to prevent seizures while closely monitoring his neurological status.
When Steve tested positive for COVID-19, a 10-day isolation period was required, and Sharon could no longer be at his bedside. “He had great people caring for him, but I couldn’t be there, and that was so difficult,” she said. “I felt very lucky that some of the medical professionals would put me on video calls so I could see him.”
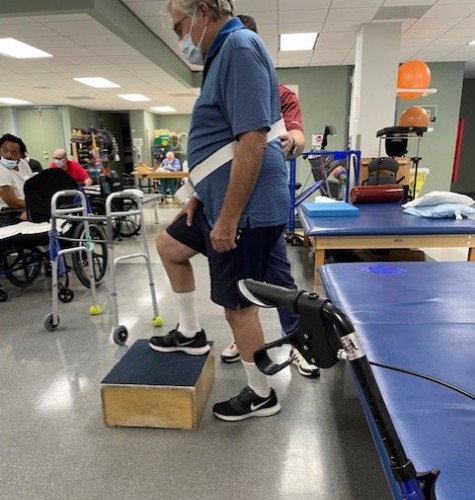
Stroke Rehabilitation Close to Home
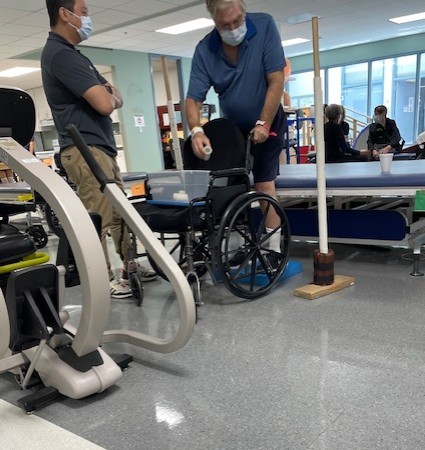
After stabilization, Steve transitioned to inpatient stroke rehabilitation at Memorial Hermann Rehabilitation Hospital-Katy, part of the Memorial Hermann Rehabilitation Network, backed by the specialists at TIRR Memorial Hermann, one of the best rehabilitation hospitals in the nation according to U.S. News & World Report.
Sharon believes “there’s no better place to be when you need rehab services.”
Stroke rehabilitation at Memorial Hermann Rehabilitation Hospital-Katy is built on a multidisciplinary, patient-centered approach that is designed to restore independence and maximize recovery. Steve’s care included:
- Physical therapy to rebuild strength, balance and mobility
- Occupational therapy to relearn daily tasks such as eating, dressing and self-care
- Speech and cognitive therapy to improve communication, memory and processing skills
His care team continuously evaluated his progress and adjusted his personalized treatment plan to support optimal neurological recovery and long-term function.
Initially, Steve required help with nearly everything. Through intensive, structured therapy and expert clinical guidance, he made steady, measurable progress. Within six months, he was walking independently, communicating more clearly and managing daily routines with greater independence.
“All the nurses and rehab therapists were phenomenal,” Sharon was quick to say. “Every person we interacted with was absolutely amazing. They made us feel like Steve wasn’t ‘just another patient’. They treated us like family.”
"Mr. Howell's journey is a powerful example of what's possible when a patient is supported by a dedicated, multidisciplinary rehabilitation team,” says P. Jacob Joseph, MD, attending physician Memorial Hermann Rehabilitation Hospital – Katy and associate professor of Physical Medicine & Rehabilitation at McGovern Medical School at UTHealth.
“From the moment he arrived for inpatient rehabilitation, our goal was to help him reclaim his independence. Seeing his determination and support from his wife Sharon, coupled with intensive and customized therapy, lead to such significant progress was incredibly rewarding for our entire team,” says P. Jacob Joseph, MD.
Long-Term Stroke Recovery and Neurological Expertise
Today, Steve lives with vascular dementia, a condition caused by reduced blood flow to the brain that affects memory, reasoning and processing speed.
Ongoing follow-up care, cognitive exercises and long-term neurological management are essential components of stroke recovery, areas where TIRR Memorial Hermann continues to support patients beyond hospitalization.
Sharon said her husband’s condition has remained stable, thanks to consistent care and engagement. “He has had multiple years of follow-up evaluations and he practices exercises to improve cognition,” she said.
He also has taken up researching family history and is practicing Spanish, a language he was previously fluent in.
Stroke Awareness Month: The Importance of Immediate Treatment and Rehabilitation
May is Stroke Awareness Month, a time to highlight the importance of early recognition and immediate care.

Stroke remains a leading cause of disability, but outcomes improve significantly when patients receive rapid treatment at experienced stroke centers like Memorial Hermann and comprehensive rehabilitation from the Memorial Hermann Rehabilitation Network that includes TIRR Memorial Hermann and Memorial Hermann Rehabilitation Hospital-Katy BE FAST to recognize the signs of stroke.
“I would recommend Memorial Hermann to anyone who needs stroke care,” Sharon said. “If we didn’t have access to this level of care, from emergency treatment through rehabilitation, Steve wouldn’t have survived.”
“What truly sets our program apart from other rehabilitation providers is a deep integration within a comprehensive health system. This model provides a continuation of care from the emergency room and medical transportation to acute hospital care to inpatient and outpatient rehabilitation. For patients like Steve recovering from complex events like a stroke, this integration means they benefit from a cohesive team and a higher level of specialized teams, which is critical for maximizing recovery,” says Dr. Joseph.
For more information about emergency services and specialty care, visit Memorial Hermann Katy Hospital.
For more information about the rehabilitation services offered at TIRR Memorial Hermann, Memorial Hermann Rehabilitation Hospital-Katy and the Memorial Hermann Rehabilitation Network, click here.