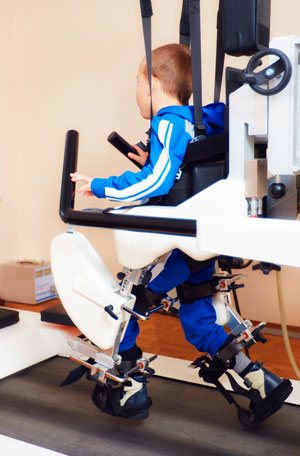
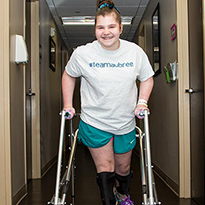
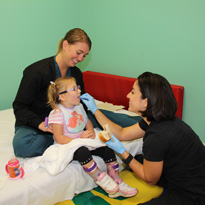
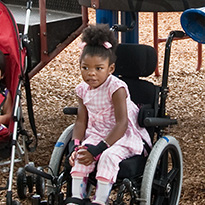Treatments range from oral medications – the least invasive – to select dorsal rhizotomy, and depend on the child’s specific condition.
Treatments range from oral medications – the least invasive – to select dorsal rhizotomy, and depend on the child’s specific condition.
Oral baclofen or muscle relaxants relax stiff or contracted muscles but may not always be effective. Because they have side effects ranging from drowsiness and changes in blood pressure to the risk of liver damage, their use requires continuous monitoring. They’re appropriate for children who need only mild improvement in muscle tone or who have widespread spasticity.
Botulinum toxin (Botox®), administered by local injection, relaxes contracted muscles by keeping nerve cells from over-activating them. Muscle relaxation occurs within days and peaks after a month, with the effect of the injection lasting three to four months.
Intrathecal baclofen therapy (ITB) requires a surgically implanted programmable pump, which uses a small catheter to deliver a concentrated form of baclofen directly to the intrathecal space surrounding the spinal cord, where the medication mixes with the cerebrospinal fluid and circulates throughout the central nervous system. Because the medication is administered continuously and directly into the intrathecal space, an ITB can be effective in providing a steady relief of symptoms without the drowsiness that is normally associated with oral baclofen. Potential side effects include increased weakness, cerebrospinal fluid leaks, and the risk of infection around the device, which is implanted below the skin in the abdomen. The pump does require regular maintenance by a physician, and because it is battery powered, the pump will need to be replaced every 5 to 7 years.
For cases of severe spasticity, selective dorsal rhizotomy (SDR) is a surgical procedure recommended when more conservative treatments – physical therapy, oral medications and drug infusion – have failed to reduce spasticity. A neurosurgeon locates and selectively severs overactivated nerves at the base of the spinal column. The procedure is most commonly used to relax muscles and decrease chronic rigidity in one or both of the lower or upper limbs.
During SDR, a neurosurgeon locates and selectively severs overactivated nerves at the base of the spinal column. The procedure is most commonly used to relax muscles and decrease chronic rigidity in one or both of the lower extremities. Benefits of SDR include immediate reduction of spasticity in patients ages 2 to 40 with spastic diplegia or spastic hemiplegia and reduced risk of spinal deformities in later years. Potential side effects include sensory loss, numbness, or uncomfortable sensations in limb areas once supplied by the severed dorsal nerve rootlets. A large surgical case series (approximately 2,700 cases) showed a minimal risk of a cerebrospinal fluid leak or need for surgical fusion.
 Treatments range from oral medications – the least invasive – to select dorsal rhizotomy, and depend on the child’s specific condition.
Treatments range from oral medications – the least invasive – to select dorsal rhizotomy, and depend on the child’s specific condition.